Urinary Tract Infections & Antimicrobial Resistance

Contents
Epidemiology of UTI
Urinary tract infections (UTIs) are the most common bacterial infections encountered by primary care physicians in the United States, accounting for approximately 7 million visits and $1.6 billion in cost annually.19, 29 Because of the shorter length of the female urethra and its proximity to the rectum, UTIs are more common in women than in men—accounting for 84% of visits.13, 19 Fifty to 70% of women will have a UTI sometime during their lifetime, and 20 to 30% will have a recurrent infection.2, 14 Known risk factors for developing uncomplicated and recurrent cases of UTIs include sexual intercourse, use of spermicides, a previous UTI, a new sex partner, and a history of UTI in a first-degree female relative.19 Changes in the normal vaginal microbiome have also been recently identified as an important risk factor for UTIs.26
The prevalence of UTIs increases with age and affects 20% of women over 65 years, which is twice the prevalence in the general population.7 Pregnancy and diabetes mellitus (DM) are also associated and have an increased risk of both first-episode and recurrent UTIs, with recurrence defined as three episodes of UTI in the last 12 months or two episodes in the last 6 months. UTIs during pregnancy may also increase the risk of preeclampsia.38
UTI is also the most common bacterial infection in children and is often associated with the presence of anatomic abnormalities. Nonetheless, the diagnosis of UTI in children is often hampered by the diversity of symptoms that can range from irritability to fever and vomiting. In this young population, encopresis—soiling of underwear with stool—is associated with recurrent UTIs.30
Hospital- and healthcare facility-acquired UTI also represent significant health and economic burden. Compared with individuals who develop community-acquired UTIs, those in healthcare settings such as nursing homes are more likely to be older, to have more co-morbidities, and to have been previously treated with antimicrobial agents.1 Hospital-acquired UTIs, which are predominantly linked to the use of urinary catheters, are often polymicrobial and are more frequently caused by multiple-drug resistant uropathogens.20
Classification of UTI
UTIs are generally classified as “uncomplicated” and “complicated.” Traditionally, uncomplicated UTIs comprise episodes of acute cystitis in healthy, non-pregnant women who have no history of urinary tract abnormalities, immunocompromised disorders, or signs of systemic infection.19 More recent classifications have expanded the list to include cases of acute uncomplicated pyelonephritis, asymptomatic bacteriuria, and recurrent uncomplicated UTIs in this category.25
By default, all other UTIs are classified as complicated and refer to infections that occur in men, pregnant women, immunocompromised patients, or those who have an anatomical or functional abnormality of the urogenital tract (for example, individuals with renal stones, urinary catheters, neurogenic bladder, spinal cord injury, and renal transplantation).
Clinical Consideration for Management
Common symptoms of acute cystitis include frequency, dysuria, suprapubic pain, and hematuria. Uncomplicated cystitis is extremely rare in young men, while in elderly men, even though symptoms of acute prostatitis, such as frequency and dysuria, can be misdiagnosed as UTI, urinary-tract obstruction resulting from prostatic edema can increase the risk of UTI.13
The prevalence of asymptomatic bacteriuria (ASB), defined as a positive urine culture with at least 105 cfu/ml collected from someone without symptoms, is reported to be between 1-5% in healthy women, 12-26% in women with DM (also increased in men with DM), and over 20% in the elderly.13 However, treatment of ASB is generally reserved for specific populations at risk for serious complications, such as renal transplant patients and pregnant women.13, 16, 23, 27 During pregnancy, ASB is associated with an increased risk of preterm delivery and a 20 to 30-fold increased risk of pyelonephritis; furthermore, antibiotic treatment of ASB has been shown to significantly reduce these risks.35
The presence of Group B streptococcus (GBS) in the urine of pregnant women indicates vaginal colonization and, therefore, also warrants treatment. GBS is the leading cause of morbidity and mortality among infants in the United States and results from vertical transmission from mother to newborn in utero or during passage through the birth canal.34 There is no diagnostic threshold for GBS to be treated. The 2002 recommendation from the CDC stated that: “clinical microbiology labs should report any concentration of GBS detected in urine (of pregnant women).”
Pathogenesis of UTI
UTIs are caused by both Gram-negative and Gram-positive bacteria, as well as by certain fungi. The most common causative agent for both uncomplicated and complicated UTIs is uropathogenic Escherichia coli (E. coli) (UPEC). Following UPEC, causative pathogens of uncomplicated UTIs in decreasing order of prevalence include Klebsiella pneumoniae (K. pneumoniae), Staphylococcus saprophyticus (S. saprophyticus), Enterococcus faecalis (E. faecalis), Group B streptococcus (GBS), Proteus mirabilis (P. mirabilis), Pseudomonas aeruginosa (P. aeruginosa), Staphylococcus aureus (S. aureus) and Candida species.11 S. saprophyticus is a predominant cause of community acquired UTI, while S. aureus occurs more frequently in urinary-catheterized individuals and pregnant women.3, 24
In cases of complicated UTIs, UPEC is followed in prevalence by Enterococcus species, K. pneumoniae, Candida species, S. aureus, P. mirabilis, P. aeruginosa, and GBS.11 Enterococci are rarely associated with community-acquired UTI but play a prominent role in the pathogenesis of catheter-associated UTI and are among the main pathogens isolated from polymicrobial infections on the surface of indwelling urinary catheters and biliary stents.9, 10, 24
There are also several emerging, rare, misclassified, and otherwise under-reported Gram-positive pathogens of the urinary tract including Aerococcus, Corynebacterium, Actinobaculum, and Gardnerella.24
Polymicrobial UTIs often involve one or more Gram-positive bacteria that have also been shown to influence the pathogenicity of co-infecting organisms; furthermore, many of these pathogens can be easily overlooked by routine diagnostic methods.24
Diagnosis of UTI
Standard Diagnostic Tests
A diagnosis of UTI based on clinical symptoms alone is often wrong. The traditional gold standard for the diagnosis of UTI is a combination of clinical symptoms and midstream urine culture. Many laboratories define 105 colony forming units (cfu)/mL urine as the threshold. However, because this threshold misses many relevant infections, a diagnosis of UTI based on a colony a count of 103 cfu/mL, depending on the types of bacteria detected, has also been recommended A diagnosis of ASB is made when an upper limit of ≥105 cfu/mL identified in a sample of midstream urine is exceeded on two consecutive occasions for women and one for men in someone without clinical symptoms of a UTI.33
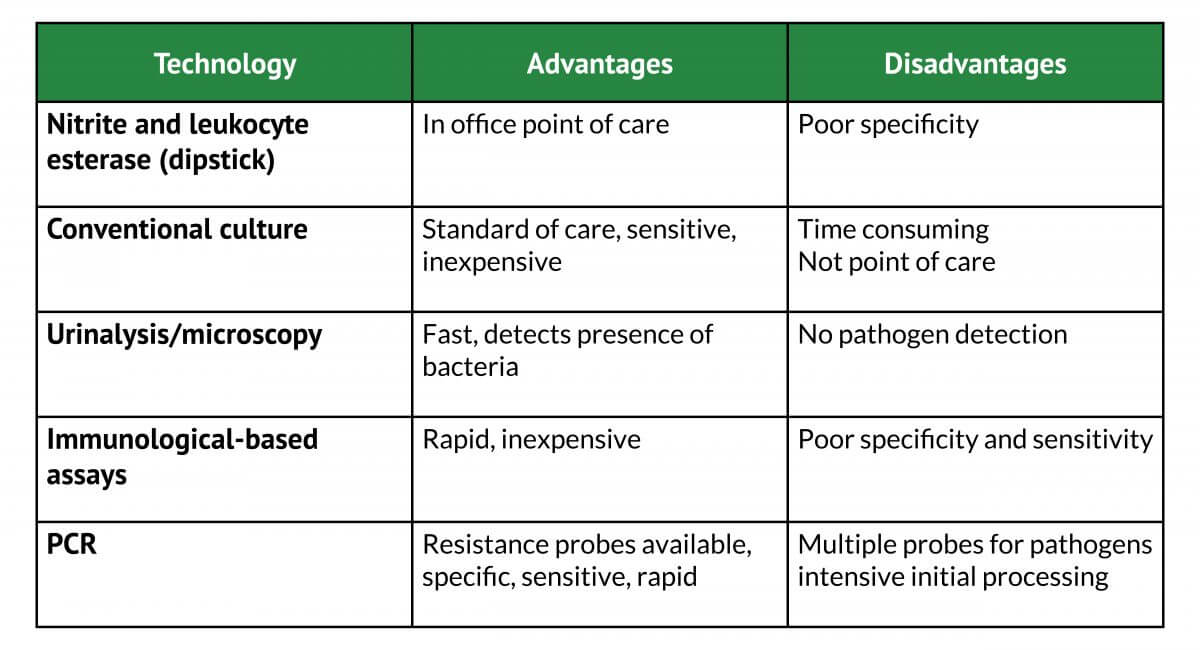
Several other diagnostic methods have both advantages and disadvantages (Table 1).36 These include: 1) dipstick, a quick method that helps identify UTIs caused by Gram-negative bacteria, but less useful for Gram-positive pathogens, especially in pregnant women and in the elderly24 2) Urine microscopy Gram-stain; 3) Immersion culture; and 4) Algorithms, where a diagnosis is based on meeting a certain number of criteria.33 In addition, new and emerging technologies are under current development.8
Tests with low specificities that lead to a high rate of false positives contribute to unnecessary prescriptions and increase the risk of resistant pathogens.
PCR
PCR-based molecular testing has been shown to be non-inferior to urine culture for detecting bacterial pathogens in symptomatic patients. In a study evaluating 582 patients with symptoms of lower UTI, in 22% (130/582) of cases, PCR was positive while culture was negative, while in only 4% (21/582) was the culture positive when the PCR was negative. Of the 30% (175/582) of patients with polymicrobial infections, 166 were reported by PCR and 39 with culture. Furthermore, polymicrobial infections were identified in 67 patients (12%, 67/582) whose culture results were negative. Thus, PCR was more accurate than culture in detecting pathogens and identified bacteria in 36% of patients who had a negative traditional urine culture. PCR was also much more sensitive than culture in detecting polymicrobial infections. This study suggests that PCR testing is more accurate and faster than traditional urine culture and also has the potential to identify polymicrobial infections with complicated mechanisms of antimicrobial resistance sharing.37
Table 1 – Comparison of technologies for UTI pathogen detection8
The Problem of Antimicrobial Resistance
Currently, antibiotics such as trimethoprim, sulfamethoxazole, ciprofloxacin, and ampicillin are the most commonly recommended drugs for treating UTIs.11 However, increasing rates of antibiotic resistance and high recurrence rates are steadily increasing the burden on our healthcare systems.
Antibiotic resistance has been well documented for members of the family Enterobacteriaceae, including E. coli and K. pneumoniae. Both pathogens have acquired plasmids encoding extended-spectrum β-lactamases (ESBLs). These plasmids rapidly spread resistance to third-generation cephalosporins among other antibiotics. Other Enterobacteriaceae produce the class C β-lactamases (AmpC enzymes), enzymes that work against cephamycin and third-generation cephalosporins; they are also resistant to β-lactamase inhibitors. The expression of AmpC enzymes is also linked to carbapenem resistance in K. pneumoniae strains.
Multidrug resistance is also common among enterococci, which are naturally resistant to trimethoprim, clindamycin, cephalosporins, and penicillins. Enterococcus species have also developed a high-level resistance to glycopeptides, including vancomycin, one of the last lines of defense against multidrug-resistant organisms.4, 6, 12, 15, 31, 32
Even though antibiotic resistance in S. saprophyticus is uncommon, methicillin-resistance has been found in ~1–8% of urine isolates and appears to be due to the acquisition of a penicillin-binding protein that has low β-lactam affinity encoded by the mecA gene. The majority of S. aureus UTI isolates, which are more common in pregnant women and catheterized individuals, are methicillin-resistant.17, 18, 22, 24, 28
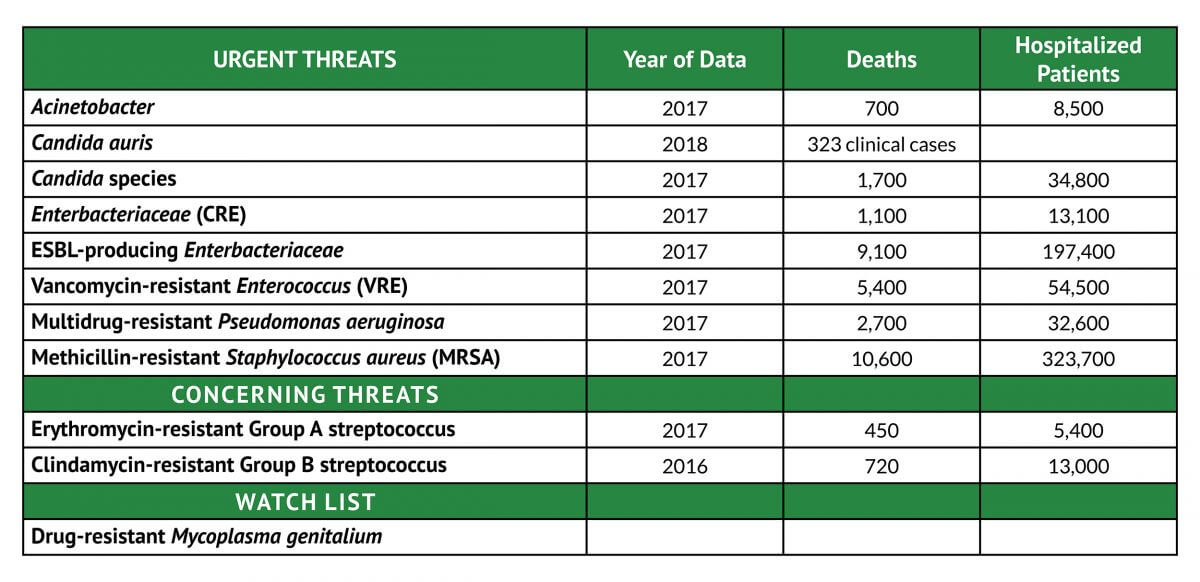
Antibiotic resistance is a global problem that is one of the biggest health challenges facing medicine today. In March 2020, the Center for Disease Control (CDC) and Prevention launched a National Action Plan to slow the emergence and spread of resistant bacteria (Tables 2 & 3). This multi-strategic plan includes heightened surveillance, education, and preventive measures, the development of new therapeutics such as vaccines, as well as the development and use of rapid and innovative diagnostic tests to identify and characterize resistant bacteria. Improved diagnostic accuracy and characterization of antibiotic resistance of common UTI pathogens is an important strategy that will reduce the overuse of antimicrobial prescriptions and slow the emergence of resistant pathogens.
Table 2 – Examples of CDC-based approaches to reducing antimicrobial resistant UTI pathogens
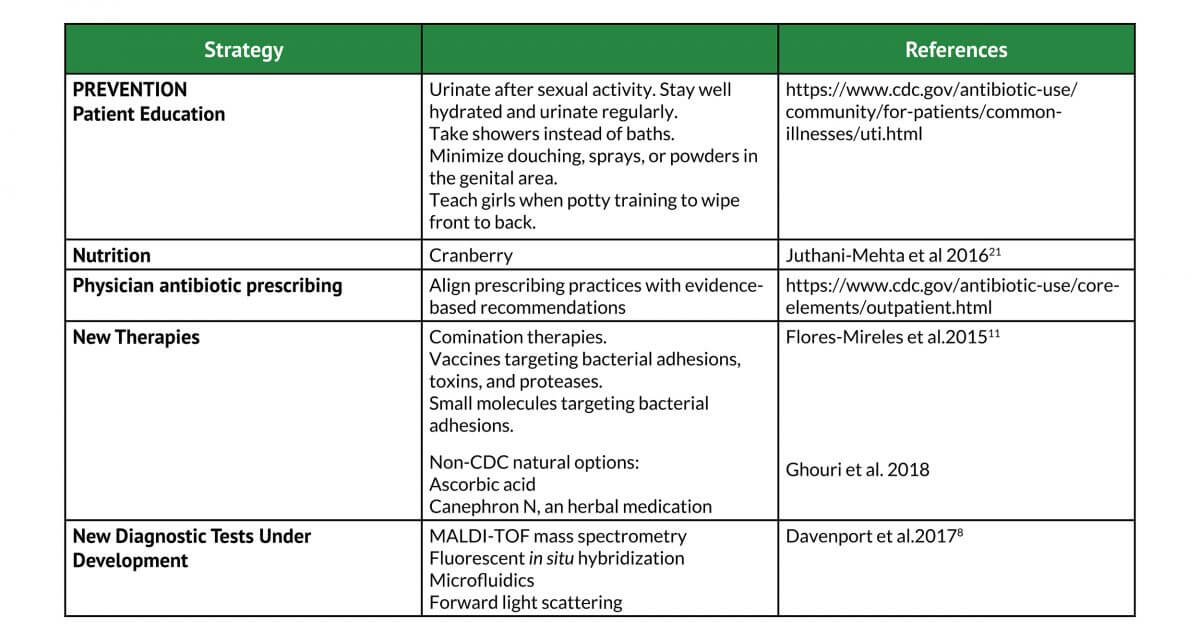
Table 3 – CDC’s Antibiotic Resistance Threats in the United States, 20195
Streamline Scientific UTI Panel
At Streamline Scientific, we provide accurate, comprehensive PCR assays for the detection of a wide range of UTI uropathogens. In addition, we offer selective antimicrobial resistance profiles to help clinicians better target therapies in an effort to reduce the use of broad therapeutic regimens that contribute to the growing threat of antibiotic resistance.
General Guidelines
Laboratory test results should always be considered in the context of clinical observations and epidemiological data (such as local prevalence rates and current outbreak/epicenter locations) in making a final diagnosis and patient management decisions. With any test, the possibility of false positive and false negative results should always be considered, and the impact on patient management decisions and clinical outcomes should be carefully weighed.
References
- Aguilar-Duran, S., et al., Community-onset healthcare-related urinary tract infections: comparison with community and hospital-acquired urinary tract infections. J Infect, 2012. 64(5): p. 478-83.
- Albert, X., et al., Antibiotics for preventing recurrent urinary tract infection in non-pregnant women. Cochrane Database Syst Rev, 2004(3): p. CD001209.
- Baraboutis, I.G., et al., Primary Staphylococcus aureus urinary tract infection: the role of undetected hematogenous seeding of the urinary tract. Eur J Clin Microbiol Infect Dis, 2010. 29(9): p. 1095-101.
- Bradford, P.A., Extended-spectrum beta-lactamases in the 21st century: characterization, epidemiology, and detection of this important resistance threat. Clin Microbiol Rev, 2001. 14(4): p. 933-51, table of contents.
- CDC drug resistance https://www.cdc.gov/drugresistance/biggest-threats.html. 2019.
- Chen, Y.H., W.C. Ko, and P.R. Hsueh, Emerging resistance problems and future perspectives in pharmacotherapy for complicated urinary tract infections. Expert Opin Pharmacother, 2013. 14(5): p. 587-96.
- Chu, C.M. and J.L. Lowder, Diagnosis and treatment of urinary tract infections across age groups. Am J Obstet Gynecol, 2018. 219(1): p. 40-51.
- Davenport, M., et al., New and developing diagnostic technologies for urinary tract infections. Nat Rev Urol, 2017. 14(5): p. 296-310.
- Dedeic-Ljubovic, A. and M. Hukic, Catheter-related urinary tract infection in patients suffering from spinal cord injuries. Bosn J Basic Med Sci, 2009. 9(1): p. 2-9.
- Desai, P.J., et al., Prevalence, identification and distribution of various species of enterococci isolated from clinical specimens with special reference to urinary tract infection in catheterized patients. Indian J Med Microbiol, 2001. 19(3): p. 132-7.
- Flores-Mireles, A.L., et al., Urinary tract infections: epidemiology, mechanisms of infection and treatment options. Nat Rev Microbiol, 2015. 13(5): p. 269-84.
- Garau, J., Other antimicrobials of interest in the era of extended-spectrum beta-lactamases: fosfomycin, nitrofurantoin and tigecycline. Clin Microbiol Infect, 2008. 14 Suppl 1: p. 198-202.
- Geerlings, S.E., Clinical Presentations and Epidemiology of Urinary Tract Infections. Microbiol Spectr, 2016. 4(5).
- Gupta, K., et al., Patient-initiated treatment of uncomplicated recurrent urinary tract infections in young women. Ann Intern Med, 2001. 135(1): p. 9-16.
- Gupta, K. and N. Bhadelia, Management of urinary tract infections from multidrug-resistant organisms. Infect Dis Clin North Am, 2014. 28(1): p. 49-59.
- Harding, G.K., et al., Antimicrobial treatment in diabetic women with asymptomatic bacteriuria. N Engl J Med, 2002. 347(20): p. 1576-83.
- Hartman, B.J. and A. Tomasz, Low-affinity penicillin-binding protein associated with beta-lactam resistance in Staphylococcus aureus. J Bacteriol, 1984. 158(2): p. 513-6.
- Higashide, M., et al., Evaluation of a cefoxitin disk diffusion test for the detection of mecA-positive methicillin-resistant Staphylococcus saprophyticus. Int J Antimicrob Agents, 2006. 27(6): p. 500-4.
- Hooton, T.M., Clinical practice. Uncomplicated urinary tract infection. N Engl J Med, 2012. 366(11): p. 1028-37.
- Hooton, T.M., et al., Diagnosis, prevention, and treatment of catheter-associated urinary tract infection in adults: 2009 International Clinical Practice Guidelines from the Infectious Diseases Society of America. Clin Infect Dis, 2010. 50(5): p. 625-63.
- Juthani-Mehta, M., et al., Effect of Cranberry Capsules on Bacteriuria Plus Pyuria Among Older Women in Nursing Homes: A Randomized Clinical Trial. JAMA, 2016. 316(18): p. 1879-1887.
- Kahlmeter, G. and Eco.Sens, An international survey of the antimicrobial susceptibility of pathogens from uncomplicated urinary tract infections: the ECO.SENS Project. J Antimicrob Chemother, 2003. 51(1): p. 69-76.
- Kim, S.J., et al., Asymptomatic Bacteriuria in Pregnancy Complicated by Pyelonephritis Requiring Nephrectomy. Case Rep Obstet Gynecol, 2018. 2018: p. 8924823.
- Kline, K.A. and A.L. Lewis, Gram-Positive Uropathogens, Polymicrobial Urinary Tract Infection, and the Emerging Microbiota of the Urinary Tract. Microbiol Spectr, 2016. 4(2).
- Kranz, J., et al., The 2017 Update of the German Clinical Guideline on Epidemiology, Diagnostics, Therapy, Prevention, and Management of Uncomplicated Urinary Tract Infections in Adult Patients. Part II: Therapy and Prevention. Urol Int, 2018. 100(3): p. 271-278.
- Lewis, A.L. and N.M. Gilbert, Roles of the vagina and the vaginal microbiota in urinary tract infection: evidence from clinical correlations and experimental models. GMS Infect Dis, 2020. 8: p. Doc02.
- Macejko, A.M. and A.J. Schaeffer, Asymptomatic bacteriuria and symptomatic urinary tract infections during pregnancy. Urol Clin North Am, 2007. 34(1): p. 35-42.
- Matsuhashi, M., et al., Molecular cloning of the gene of a penicillin-binding protein supposed to cause high resistance to beta-lactam antibiotics in Staphylococcus aureus. J Bacteriol, 1986. 167(3): p. 975-80.
- Medina, M. and E. Castillo-Pino, An introduction to the epidemiology and burden of urinary tract infections. Ther Adv Urol, 2019. 11: p. 1756287219832172.
- Michael, M., et al., Short versus standard duration oral antibiotic therapy for acute urinary tract infection in children. Cochrane Database Syst Rev, 2003(1): p. CD003966.
- Paterson, D.L., Resistance in gram-negative bacteria: Enterobacteriaceae. Am J Infect Control, 2006. 34(5 Suppl 1): p. S20-8; discussion S64-73.
- Pendleton, J.N., S.P. Gorman, and B.F. Gilmore, Clinical relevance of the ESKAPE pathogens. Expert Rev Anti Infect Ther, 2013. 11(3): p. 297-308.
- Schmiemann, G., et al., The diagnosis of urinary tract infection: a systematic review. Dtsch Arztebl Int, 2010. 107(21): p. 361-7.
- Verani, J.R., et al., Prevention of perinatal group B streptococcal disease–revised guidelines from CDC, 2010. MMWR Recomm Rep, 2010. 59(RR-10): p. 1-36.
- Verma, A., S. Baheti, and M. Sharma, Asymptomatic bacteriuria in pregnancy and its relation. Int J Reprod Contracept Obstet Gynecol, 2016. 5(12): p. 4390-4396.
- Wilson, M.L. and L. Gaido, Laboratory diagnosis of urinary tract infections in adult patients. Clin Infect Dis, 2004. 38(8): p. 1150-8.
- Wojno, K.J., et al., Multiplex PCR Based Urinary Tract Infection (UTI) Analysis Compared to Traditional Urine Culture in Identifying Significant Pathogens in Symptomatic Patients. Urology, 2020. 136: p. 119-126.
- Yan, L., et al., The association between urinary tract infection during pregnancy and preeclampsia: A meta-analysis. Medicine (Baltimore), 2018. 97(36): p. e12192.
Ready to take charge of your lab
services?
START YOUR LAB
USE OUR LAB
© Copyright 2026 | All Rights Reserved | Privacy Policy | Terms of Use | Do not sell or share my personal information